Quality of Life Innovations from the Columbia University Department of Surgery
Advances in Breast Cancer Surgery
Nipple-sparing mastectomy allows women to maintain normal breast
appearance after surgery.
Clinical Breast Cancer Program
Columbia University Medical Center
800-227-2762
Advances in Breast Cancer Surgery
Nipple-sparing mastectomy allows women to maintain normal breast
appearance after surgery.
Clinical Breast Cancer Program
Columbia University Medical Center
800-227-2762
| The New York Optimist |
SHARE
| © MMIX, The New York Optimist. All Rights Reserved. The New York Optimist & www.thenewyorkoptimist.com is a registered trademark of The New York Optimist. The New York Optimist is a registered service mark of Thenewyorkoptimist.com. The New York Optimist logo and original photos are a registered trademark of The New York Optimist . All other photos are property of the advertiser. And are rightfully protected under their copywright protections. |
Most breast cancer patients who require surgery today
(75%) can undergo breast conservation (lumpectomy) rather
than mastectomy (removal of the entire breast). Yet many
women still require or choose to undergo mastectomy, either
to treat or prevent breast cancer. Such patients may have
cancer in multiple areas of the breast, or be healthy but have
the BRCA gene, which puts them at high risk of developing
breast cancer.
(75%) can undergo breast conservation (lumpectomy) rather
than mastectomy (removal of the entire breast). Yet many
women still require or choose to undergo mastectomy, either
to treat or prevent breast cancer. Such patients may have
cancer in multiple areas of the breast, or be healthy but have
the BRCA gene, which puts them at high risk of developing
breast cancer.
Mastectomy has evolved dramatically from the early days, in which removal of the breast, all axillary lymph nodes, and chest wall
muscle often left women with swollen arms, chest wall deformity, and a negative body image after surgery. In the 1970's radical
mastectomy gave way to a modified form of surgery, in which the breast tissue and lymph nodes were removed but the chest muscle
was left intact. Breast reconstruction was infrequently performed at that time. Technique advanced further with lumpectomy, in
which the breast could be preserved by excising the cancer with a surrounding margin of normal tissue. During the early 1990's, a
skin-sparing mastectomy was developed in which the nipple-areola area was removed with a central incision, breast tissue removed
through that space, and the skin envelope used to rebuild the breast (using the patient's own body tissue or an implant). "This was a
major improvement in technique," says Sheldon Feldman, MD, Chief, Breast Surgery Division.
muscle often left women with swollen arms, chest wall deformity, and a negative body image after surgery. In the 1970's radical
mastectomy gave way to a modified form of surgery, in which the breast tissue and lymph nodes were removed but the chest muscle
was left intact. Breast reconstruction was infrequently performed at that time. Technique advanced further with lumpectomy, in
which the breast could be preserved by excising the cancer with a surrounding margin of normal tissue. During the early 1990's, a
skin-sparing mastectomy was developed in which the nipple-areola area was removed with a central incision, breast tissue removed
through that space, and the skin envelope used to rebuild the breast (using the patient's own body tissue or an implant). "This was a
major improvement in technique," says Sheldon Feldman, MD, Chief, Breast Surgery Division.
Nipple-sparing mastectomy originated about fifteen years ago in Japan, where surgeons developed the procedure and reported
excellent results. Dr. Feldman traveled to Japan in 2004 to learn the procedure, and then began performing it in 2005. Dr.
Ananthakrishnan gained expertise in nipple-sparing mastectomy while at the Cleveland Clinic, before accepting her faculty
appointment at NewYork-Presbyterian/Columbia this year.
excellent results. Dr. Feldman traveled to Japan in 2004 to learn the procedure, and then began performing it in 2005. Dr.
Ananthakrishnan gained expertise in nipple-sparing mastectomy while at the Cleveland Clinic, before accepting her faculty
appointment at NewYork-Presbyterian/Columbia this year.
Drs. Feldman, Ananthakrishnan and Taback work closely with surgeons in the Division of Plastic Surgery (Drs. Ascherman, Grant
and Rohde), whose collaboration is critical during such procedures. In some cases, the plastic surgeon will place a tissue expander
under the muscle at the time of mastectomy, in preparation for a final implant at a later time. Alternatively, fatty tissue from the
abdomen can be used to replace the removed breast tissue by performing a TRAM or DIEP flap. Many women prefer the tissue flap
techniques because they get a “tummy tuck” procedure when extra fatty tissue from the abdomen is removed to create a new breast.
and Rohde), whose collaboration is critical during such procedures. In some cases, the plastic surgeon will place a tissue expander
under the muscle at the time of mastectomy, in preparation for a final implant at a later time. Alternatively, fatty tissue from the
abdomen can be used to replace the removed breast tissue by performing a TRAM or DIEP flap. Many women prefer the tissue flap
techniques because they get a “tummy tuck” procedure when extra fatty tissue from the abdomen is removed to create a new breast.
Dr. Ananthakrishnan is enthusiastic about offering nipple-sparing mastectomy at NYP/Columbia. "We practice with a team approach,
meaning the patient meets with the breast surgical oncologist and the plastic surgeon prior to surgical planning. By working as a team,
we are able to optimize both the treatment of the cancer as well as the aesthetic outcome after surgery."
For more information, visit www.breastmd.org
meaning the patient meets with the breast surgical oncologist and the plastic surgeon prior to surgical planning. By working as a team,
we are able to optimize both the treatment of the cancer as well as the aesthetic outcome after surgery."
For more information, visit www.breastmd.org
Meanwhile, plastic and reconstructive surgeons developed techniques to reconstruct the breast during the mastectomy
(rather than months or years later). Although controversial at first, immediate breast reconstruction has been shown to be
safe. The advancement of oncoplastic techniques allows many women today to emerge from mastectomy with a more natural
appearance, while still receiving optimal treatment for their cancer.
(rather than months or years later). Although controversial at first, immediate breast reconstruction has been shown to be
safe. The advancement of oncoplastic techniques allows many women today to emerge from mastectomy with a more natural
appearance, while still receiving optimal treatment for their cancer.
Today, however, an even better option is now available: it is possible to perform mastectomy while retaining not only the skin,
but also the nipple and areola complex. "If there is no cancer in the area of the nipple or areola, this tissue can be
preserved," explains Preya Ananthakrishnan, MD, Assistant Professor of Clinical Surgery and Associate Director, Breast
Surgery Fellowship. Along with Dr. Feldman and Bret Taback, MD Assistant Professor of Surgery and Director, Breast
Surgical Oncology Fellowship Program, Dr. Ananthakrishnan specializes in nipple-sparing mastectomy and onplastic surgery
for women with breast cancer. "In order to preserve the skin, nipple, and areola, we perform mastectomy by making very
small incisions under the breast or on the side of the breast. Keeping all of the skin envelope preserves the shape of their
breasts most naturally, which provides the best possible cosmetic outcome."
but also the nipple and areola complex. "If there is no cancer in the area of the nipple or areola, this tissue can be
preserved," explains Preya Ananthakrishnan, MD, Assistant Professor of Clinical Surgery and Associate Director, Breast
Surgery Fellowship. Along with Dr. Feldman and Bret Taback, MD Assistant Professor of Surgery and Director, Breast
Surgical Oncology Fellowship Program, Dr. Ananthakrishnan specializes in nipple-sparing mastectomy and onplastic surgery
for women with breast cancer. "In order to preserve the skin, nipple, and areola, we perform mastectomy by making very
small incisions under the breast or on the side of the breast. Keeping all of the skin envelope preserves the shape of their
breasts most naturally, which provides the best possible cosmetic outcome."
"The ability to keep the entire breast skin, nipple and areola makes for a far gentler mastectomy," says Dr. Ananthakrishnan.
"For some women, this makes a very important difference in their experience with surgery and overall healing." Not all patients
are eligible for this procedure; biospies are performed during surgery to make sure that the nipple is cancer-free.
"For some women, this makes a very important difference in their experience with surgery and overall healing." Not all patients
are eligible for this procedure; biospies are performed during surgery to make sure that the nipple is cancer-free.
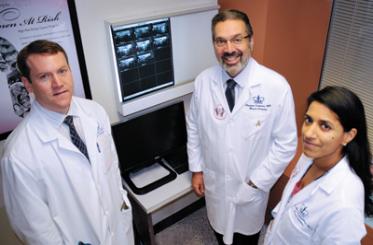
Bret Taback, MD, Assistant Professor of Surgery and Director, Breast Surgical
Oncology Fellowship Program; Sheldon Feldman, MD, Vivian L. Milstein
Associate Professor of Clinical Surgery and Chief, Breast Surgery Division;
and Preya Ananthakrishnan, MD, Assistant Professor of Clinical Surgery and
Associate Director, Breast Surgery Fellowship.
Oncology Fellowship Program; Sheldon Feldman, MD, Vivian L. Milstein
Associate Professor of Clinical Surgery and Chief, Breast Surgery Division;
and Preya Ananthakrishnan, MD, Assistant Professor of Clinical Surgery and
Associate Director, Breast Surgery Fellowship.